The Value of Time in Medicine

How Delays Change Diagnosis, Treatment Scope, and Clinical Outcomes, and Why Patient Routing Is of Key Importance
In medicine, time is rarely measured in calendar terms. It is measured by changes in the clinical picture, diagnostic complexity, the scope of required treatment, and the consequences for the patient's quality of life. In many cases, time determines not only the prognosis but also how early and accurately a diagnosis will be established, as well as how appropriate the chosen treatment strategy will be.
At the same time, delay does not always appear as a lack of care. More often, the patient is in the process of treatment, observation, or repeated consultations. However, the most important element may be missing: a structured medical trajectory. This is not about the speed of scheduling a doctor's appointment, but about the sequence of clinical decisions: who should assess the situation first, which tests are truly necessary, which diagnoses should be ruled out as a priority, and at what stage it is appropriate to involve a specialized center.
In practice, time is most often lost in several typical scenarios.
- When symptoms are interpreted as typical or age-related and are explained by the same hypothesis for an extended period.
- When examinations are conducted in a fragmented manner, without a clear understanding of the diagnostic goal.
- When the patient ends up with a non-specialized physician or in a medical facility where such cases are not addressed systematically.
In such situations, a patient may remain in a state of uncertainty for years. Symptoms persist or worsen, while the true cause of the disease remains unidentified. In a number of medical fields, including urology, oncology, and orthopedics, such delays directly affect the complexity of subsequent treatment and its scope.
What Is Meant by Proper Patient Routing
Patient routing is medical navigation built on clinical logic. It involves a sequence of actions where each stage answers a specific diagnostic or treatment question. This approach helps avoid both unjustified delays and hasty decisions made without sufficient diagnostic workup.
In the German healthcare system, this principle is implemented through interdisciplinary collaboration. In university hospitals and specialized centers, complex clinical cases are reviewed with the participation of specialists from different fields. This reduces the likelihood of diagnostic errors and allows for an assessment of the patient's condition as a whole, rather than within the framework of a single narrow specialty.
Clinical Case from German Medical Concierge Practice
In our practice, we frequently encounter situations where a patient has been under observation for a long time, receiving treatment, yet the underlying cause of the condition remains unidentified.
A 66-year-old man had been experiencing recurrent urological inflammations for nearly ten years. The symptoms were recurrent and partially managed, which created the impression of a chronic but non-critical problem. As a result, the condition was not considered to require in-depth diagnostics, and observation was limited to symptomatic treatment.
After another episode of exacerbation, the patient finally sought medical consultation. A blood test for prostate-specific antigen was significantly elevated and became the basis for further examination, including magnetic resonance imaging of the prostate. The preliminary results raised serious clinical concerns and required further verification.
At this stage, the patient contacted German Medical Concierge. The team's task was not to formally accelerate the process, but to establish a correct clinical trajectory and engage specialized expertise. On the same day, direct communication was arranged with a urology department in Berlin specializing in prostate diseases, and an in-person consultation with a specialized physician was scheduled.
The next step was a targeted prostate biopsy followed by morphological examination. Based on the examination results, a diagnosis of prostate cancer was established.
To assess the extent of the disease, the patient underwent additional examination, including bone scintigraphy. No signs of distant metastasis were detected, which allowed for radical treatment to be considered as a justified and timely approach.
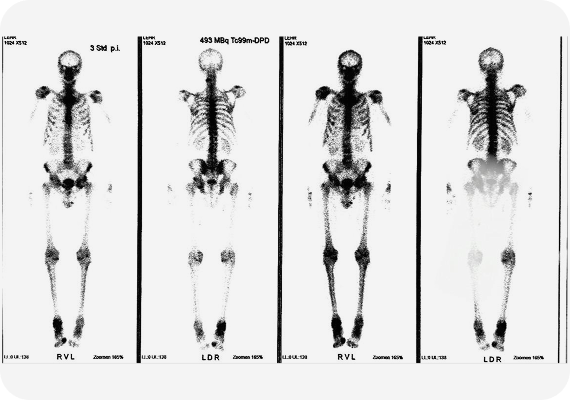
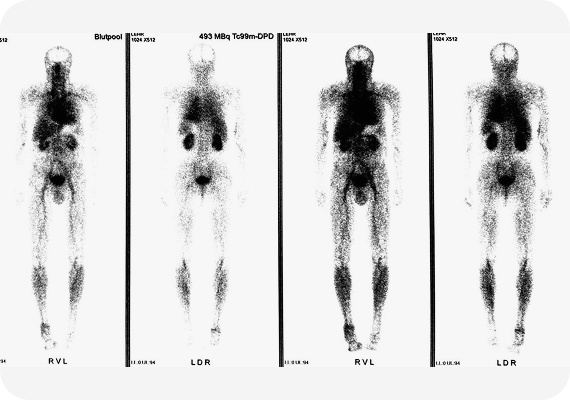
Taking into account the stage of the disease, clinical data, and the patient's overall condition, a surgical treatment strategy was determined. The choice of intervention method was made based on medical indications, with the goal of a maximally sparing approach while preserving oncological radicality.
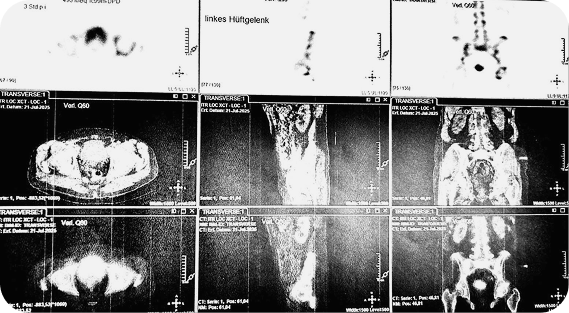
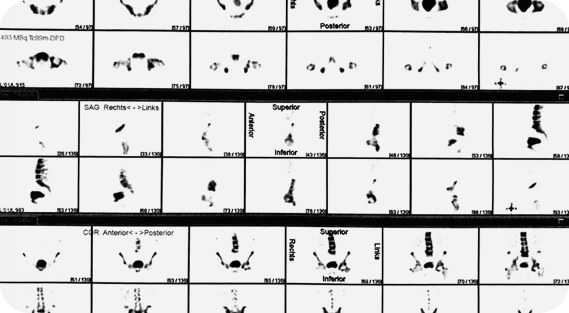
Growing Demand for Treatment in Germany in the Region
The entire journey, from the initial contact with German Medical Concierge to the clinical decision and preparation for surgery, took approximately two and a half weeks. Without clear routing, such cases often drag on for months, which can lead to an increase in treatment scope and complicate the clinical course of the disease.

This example clearly demonstrates that in complex clinical situations, the decisive factor is not only the level of medical technology, but also the timely involvement of appropriate expertise, the consistency of diagnostic steps, and professional medical navigation.
The role of German Medical Concierge
The role of the team is not to replace the treating physician, but to ensure that the patient reaches the appropriate specialist, in the right medical institution, and at the optimal moment from a clinical perspective.
In complex cases, such structured navigation helps to avoid unnecessary delays, reduce periods of uncertainty, and support balanced, well-founded medical decision-making.
The value of time in medicine is measured not in days, but in consequences. Delays resulting from the absence of structured patient navigation can alter diagnosis, increase treatment scope, and complicate the patient’s clinical journey. Timely and well-coordinated navigation, by contrast, helps preserve opportunities for more accurate diagnosis and more conservative treatment approaches.
For this reason, time in medicine should be regarded as a clinical factor that requires the same level of attention as the diagnosis itself.